This test measures D-dimer in the blood. D-dimer tests are ordered along with other lab tests and imaging scans to help rule out, diagnose, and monitor a range of blood clotting conditions. It is a quick test to do and is often used as a first-line test to rule out clotting conditions – D-dimer is especially useful when your doctor thinks that something other than a major blood clot is causing your symptoms. If you have a positive D-dimer test result you will need other tests to find out the cause. If you have a negative result, it is unlikely that you have abnormal blood clotting.
What is being tested?
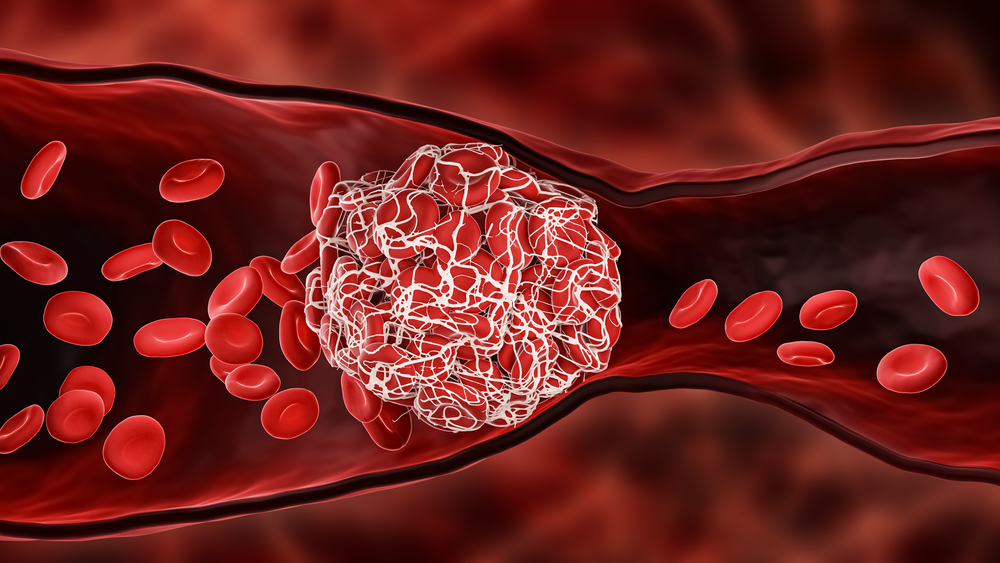
When a vein or artery is injured and begins to leak blood, a sequence of clotting steps and factors (called the coagulation cascade) is activated by the body to limit the bleeding and create a blood clot to plug the hole. During this process, threads of a protein called fibrin are produced. These threads are crosslinked (glued together) to form a fibrin net that catches platelets and helps hold the forming blood clot together at the site of the injury.
Once the area has had time to heal, the body uses a protein called plasmin to break the clot (thrombus) into small pieces so that it can be removed. The fragments of the disintegrating fibrin in the clot are called fibrin degradation products (FDP). One of the FDPs produced is D-dimer, which consists of variously sized pieces of crosslinked fibrin. D-dimer is normally undetectable in the blood and is produced only after a clot has formed and is in the process of being broken down. Measurement of D-dimer can tell your doctor that something has increased the body's clotting mechanisms above its normal limits.
How is it used?
D-dimer tests are ordered, along with other laboratory tests and imaging scans, to help rule out, diagnose, and monitor diseases and conditions that cause hypercoagulability, a tendency to clot inappropriately. One of the most common of these conditions is DVT (deep vein thrombosis), which involves clot formation in the deep veins of the body, most frequently in the legs. These clots may grow very large and block blood flow in the legs, causing swelling, pain, and tissue damage. It is possible for a piece of the clot to break off (this broken piece is called an embolus) and travel to other parts of the body, where the clot can cause a PE (pulmonary embolus or embolism - blood clot in the lungs).
While clots most commonly form in the veins of the legs, they may also form in other areas as well; for example, clots in coronary arteries are the cause of myocardial infarction (heart attacks). Clots may also form on the lining of the heart or its valves, particularly when the heart is beating irregularly (atrial fibrillation) or when the valves are damaged. Clots also may form in large arteries as a result of damage from atherosclerosis (sometimes called hardening of the arteries). Pieces of such clots may also break off and cause an embolus that blocks an artery in another organ, such as the brain (causing a stroke) or the kidneys. Measurements of D-dimer can also be used to detect clots in these other sites.
Measurements of D-dimer may also be ordered, along with other tests, to help diagnose DIC (disseminated intravascular coagulation). DIC is a complex acute condition that can arise from a variety of situations including: some surgical procedures, septic shock, poisonous snake bites, liver disease, and postpartum (after the delivery of a baby). With DIC, clotting factors are activated and then used up throughout the body. This creates numerous minute blood clots and at the same time leaves the patient vulnerable to excessive bleeding. Steps are taken to support the patient, while the underlying problem is addressed, and the underlying condition resolved. D-dimer levels may be used to monitor the effectiveness of DIC treatment.
When is it requested?
D-dimer may be ordered when a patient has symptoms of DVT, such as leg pain, tenderness, swelling, discoloration, oedema; or symptoms of PE, such as laboured breathing, coughing, and lung-related chest pain. D-dimer is especially useful when the doctor thinks that something other than DVT or PE is causing the symptoms. It is a quick, non-invasive way for the doctor to help rule out abnormal or excess clotting.
When a patient has symptoms of DIC, such as bleeding gums, nausea, vomiting, severe muscle and abdominal pain, seizures and oliguria (decreased urine output), a D-dimer test may be ordered, along with a PT, APTT, fibrinogen and platelet count to help diagnose the condition. D-dimer may also be ordered at intervals when a patient is undergoing treatment for DIC to help monitor its progress.
What does the result mean?
A positive D-dimer indicates the presence of an abnormally high level of fibrin degradation products in your body. It tells your doctor that there has been significant clot (thrombus) formation and breakdown in the body, but it does not tell the location or cause. An elevated D-dimer may be due to a venous thromboembolism (VTE) or DIC but it may also be due to a recent surgery, trauma or infection. Elevated levels are also seen with liver disease, pregnancy, eclampsia, heart disease, and some cancers.
A normal D-dimer test means that it is most likely that you do not have an acute condition or disease that is causing abnormal clot formation and breakdown. Most doctors agree that a negative D-dimer is most valid and useful when the test is done on patients that are considered to be low-risk. The test is used to help rule out clotting as the cause for the symptoms.
D-dimer is recommended as an adjunct additional test. It should not be the only test used to diagnose a disease or condition. Both increased and normal D-dimer levels may require follow-up and can lead to further testing.
Is there anything else I should know?
Anticoagulant therapy can cause a false negative D-dimer. There are several different methods of testing for D-dimer. Most of the D-dimer tests that yield quantitative results are done in a hospital laboratory, while those that yield qualitative results are performed at the patient’s bedside. D-dimer concentrations may rise in the elderly, and false positives may be seen with high levels of rheumatoid factor (a protein seen in patients with rheumatoid arthritis).
Substances such as high triglycerides, lipaemia (a large amount of fats in the blood that can be caused by the patient consuming a greasy meal prior to testing), and bilirubin can also cause false positives as can haemolysis caused by improper sample collection and handling.
Common questions
At the present time, there is no FDA approved D-dimer test for home use.
More than likely, your doctor will order a non-invasive scanning procedure, such as a venous ultrasound. Additional procedures may include ventilation/perfusion or a CT scan.
More information
What is Pathology Tests Explained?
Pathology Tests Explained (PTEx) is a not-for profit group managed by a consortium of Australasian medical and scientific organisations.
With up-to-date, evidence-based information about pathology tests it is a leading trusted source for consumers.
Information is prepared and reviewed by practising pathologists and scientists and is entirely free of any commercial influence.